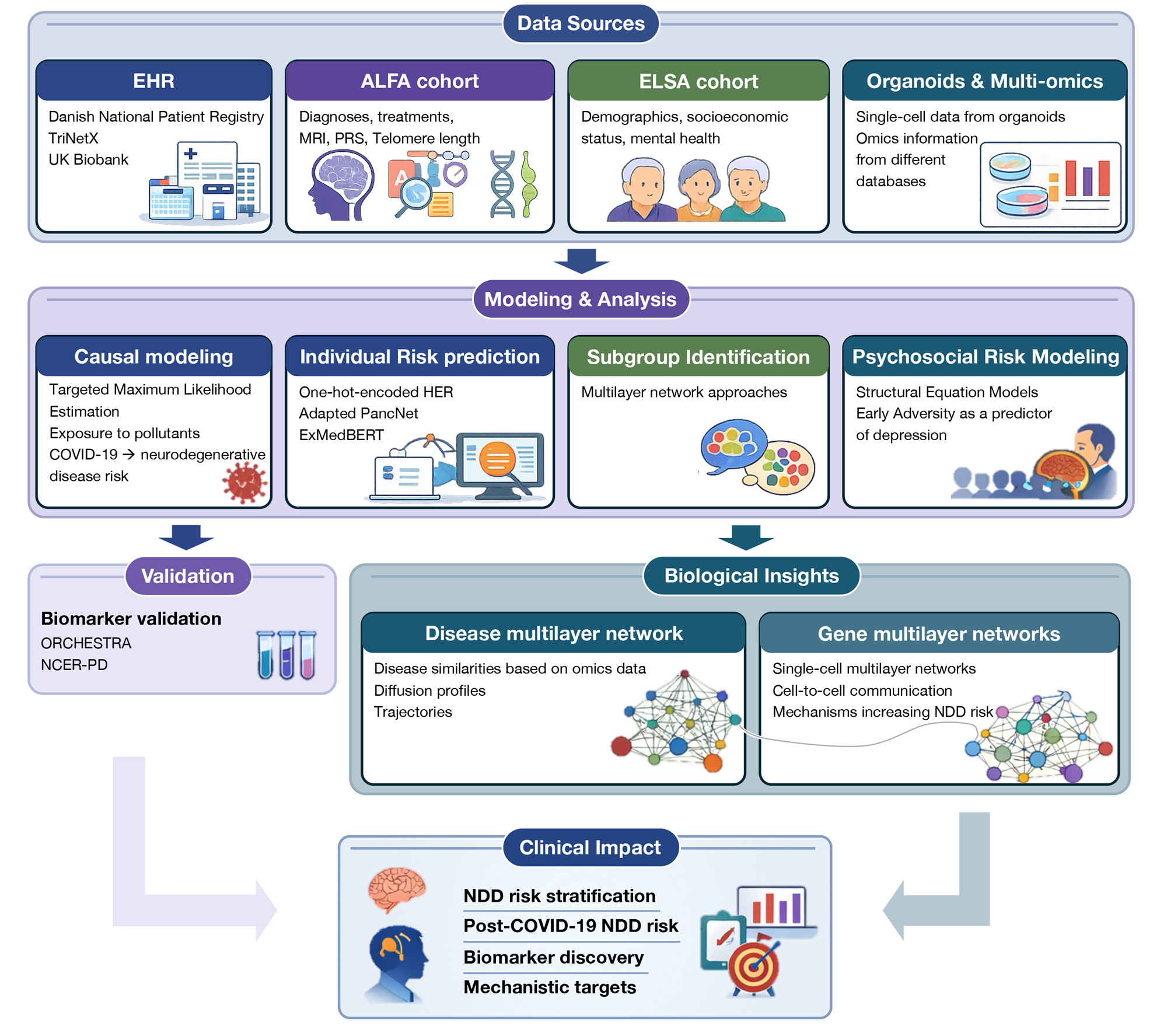
Risk modelling using real-world health data
WP3 analyses large Electronic Health Record (EHR) datasets including the UK Biobank, IBM Explorys, TriNetX, and the Danish National Patient Registry.
Using these resources, the team develops complementary modelling approaches:
Population-level causal models estimate the effect of COVID-19 infection on later neurodegenerative disease diagnoses across populations and subgroups. These models help reduce bias in observational data and improve the design of longitudinal risk prediction studies.
Individualised risk prediction models estimate how a person’s risk of neurodegenerative disease may change depending on whether they have experienced COVID-19 infection. Medical histories are analysed using machine learning techniques, including transformer-based models.
To understand how predictions are made, explainability tools are used to identify the clinical and demographic factors that most strongly influence risk.
Psychosocial and life-course risk
WP3 also examines how social and life-course factors interact with COVID-19 exposure to influence mental health and cognitive outcomes.
Using data from the English Longitudinal Study of Ageing (ELSA), researchers analyse how early-life adversity relates to later-life depression and cognitive decline in the context of the pandemic.
Initial findings suggest that early-life disadvantage can have long-term effects on mental health, with different types of deprivation affecting depression and cognition in different ways.
Future analyses will compare results across European cohorts to assess how consistent these patterns are across populations.
Multimodal risk stratification
Deeply characterised research cohorts, such as the ALFA cohort, are used to identify individuals who may have increased Alzheimer’s disease risk related to COVID-19.
These analyses integrate multiple data types, including:
- brain imaging
- genetic risk scores
- telomere length
- clinical information
Combining these sources allows researchers to better identify subgroups that may be particularly vulnerable to neurodegenerative processes.
Understanding biological mechanisms
To connect epidemiological findings with biology, WP3 develops multilayer network models that integrate different types of biomedical data.
These models combine information on:
- genes
- molecular pathways
- clinical symptoms
- drug targets
- microbiome and transcriptomic data
By analysing these networks, researchers can identify shared biological pathways linking COVID-19 with neurodegenerative diseases.
Potential biomarkers emerging from these analyses will be experimentally validated in collaboration with Work Package 4.
 Comorbidity Mechanisms Utilized in Healthcare
Comorbidity Mechanisms Utilized in Healthcare